When you're juggling back-to-back appointments, chasing down lab results, and fielding client calls, clear documentation can slip down the priority list. But when done right, veterinary SOAP notes keep records tidy and make the entire clinic run smoother.
SOAP stands for Subjective, Objective, Assessment, and Plan. It's the gold standard format for documenting patient visits in veterinary medicine. Whether you're dealing with a straightforward vaccine appointment or a complex lameness case, SOAP vet notes help structure your thinking, improve communication across the team, and ensure consistent, high-quality care.
The challenge? Writing them takes time. And when time is already tight, that often means catching up after hours, relying on memory, or skipping details altogether. That's where automation can make a real difference—without cutting corners.
In this article, you'll learn why SOAP vet notes matter for every veterinary role on your team, how to break down each section effectively, and where AI copilot tools like CoVet fit into your clinic workflow.
Why SOAP notes matter in veterinary practices
When every team member documents in the same structured way, it's easier to track patient progress, avoid repeat diagnostics, and make sure nothing falls through the cracks during handoffs.
But even though the format is simple, creating efficient SOAP notes isn't always easy.
Time pressure: With packed schedules, there's often little time to finish notes between appointments. Many DVMs end up documenting late into the evening or relying on rushed memory recalls.
Inconsistent documentation: Without a shared approach, records can vary dramatically between team members—making it harder to get a clear picture of the patient's history.
Missed details: When you're multitasking, it's easy to forget a minor symptom or treatment instruction. Over time, those gaps can affect care quality and follow-up decisions.
Structured SOAP vet notes help solve these problems—but only if they're used consistently, and without adding extra work. That's where our tips for SOAP writing and veterinary dictation software come in.
Breaking down the SOAP format
Each part of a SOAP note serves a clear purpose. When used consistently, the format helps your team communicate clearly, track patient changes over time, and make faster, more informed decisions. Here's how to approach each section with soap veterinary example entries you can adapt for common visits.
Section | Purpose | Example |
|---|---|---|
Subjective | Owner/team reports, history, symptoms | "Lethargic for 2 days, decreased appetite" |
Objective | Physical exam findings, vitals, lab results | T: 39.2°C, HR: 120, mild dehydration |
Assessment | Diagnosis or differential list | Suspected gastroenteritis, rule out foreign body |
Plan | Treatment, diagnostics, follow-up | IV fluids, abdominal radiographs, recheck in 24h |

Subjective: What the pet owner or team reports
This is where the visit starts. The Subjective section includes any observations shared by the client or your team—things that can't be measured directly but still offer critical context.
What to include:
Reported symptoms (vomiting, limping, appetite changes)
Behavior changes (hiding, vocalizing, aggression)
Historical details (duration of signs, response to past treatments)
Objective: What you can measure or observe
This section covers facts—anything you or your team can physically observe, measure, or test. It's the most straightforward part of the note, but getting it right is critical for tracking trends and supporting your assessment.
Parameter | What to Record | Why It Matters |
|---|---|---|
Temperature | Rectal temp in °C or °F | Detects fever, hypothermia |
Heart rate | Beats per minute, rhythm | Cardiovascular assessment |
Respiratory rate | Breaths per minute, effort | Respiratory function |
Weight | Current weight, trend over visits | Dosing, nutritional status |
Body condition score | BCS on 1–9 scale | Nutritional assessment |
Hydration status | Skin turgor, mucous membranes | Fluid therapy decisions |
Assessment: What's the diagnosis or problem list?
This is where clinical reasoning comes in. The Assessment section summarizes your interpretation of the case so far. It might be a confirmed diagnosis, a list of differentials, or a note about ongoing monitoring.
Plan: What happens next?
The Plan outlines what you're doing about the problem. This includes treatments, diagnostics, client communication, and follow-up instructions. It should be actionable and easy for the rest of the team to follow.
Category | Example | Notes |
|---|---|---|
Medication | Rimadyl 2mg/kg PO BID × 7 days | Include dose, route, frequency, duration |
Diagnostics | Abdominal radiographs (2 views) | Specify views, urgency |
Surgery | Schedule dental prophylaxis | Include pre-op instructions |
Client education | Diet transition handout provided | Document what was discussed |
Follow-up | Recheck in 10–14 days | Specify timeline and purpose |
How CoVet helps automate SOAP note-taking
Even when you know what a great SOAP note looks like, writing them during a packed clinic day is another story. CoVet steps in—not as a replacement, but as a second set of hands that never misses a detail.
Real-time voice capture
CoVet listens as you talk—during or after the appointment—and automatically generates draft notes in the proper SOAP format. You don't need to repeat yourself or summarize after the fact. Just speak naturally, and the AI handles the structure.
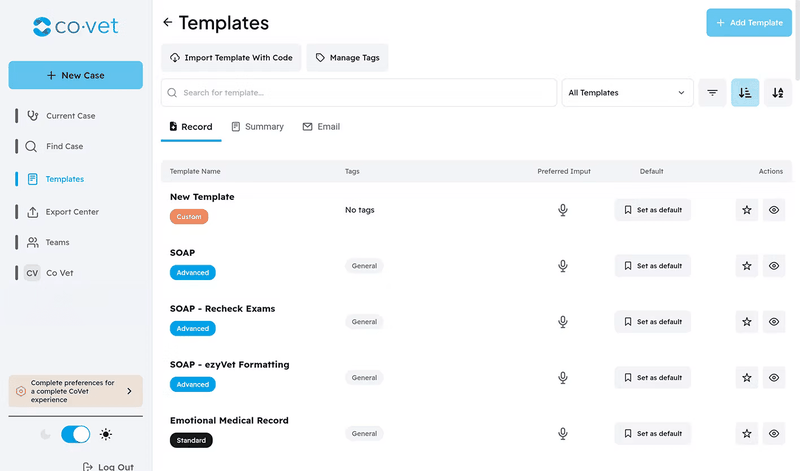
Role-specific customization
Whether you're a DVM, technician, or client care specialist, CoVet adapts to your role. You get what you need—without being overwhelmed by details that aren't relevant to your part of the case.
Built-in PIMS integration
No double entry, no extra tabs. CoVet syncs directly with your practice management software, so finalized notes go exactly where they belong.
Standardization across the team
By guiding everyone to document using the same structure and language, CoVet helps reduce variability in records. That means fewer follow-up calls, better compliance, and smoother team handoffs.
Details don't get dropped
When notes are created in real time, you capture more nuance. That builds client trust, supports better medicine, and helps keep the whole care team aligned.
Better documentation for every care team
In a busy general practice, it's easy for documentation to become an afterthought. But SOAP notes aren't just for compliance. They're a tool to deliver better medicine, reduce miscommunication, and protect your time. When they're structured and consistent, your whole team benefits.
With CoVet, you don't need to trade off between quality and speed. By automating the SOAP process and integrating directly with your PIMS, CoVet helps you capture accurate, complete records—right when the care is happening. That means fewer late nights, fewer missed details, and more time for what actually matters: the patient in front of you.
About the Author
Iain MacNeil
Co-founder and CEO at CoVet. Veterinary professional and technology enthusiast committed to reducing administrative burden for veterinary teams worldwide.
)
)
)
